How can we help?
We are here to connect, listen, empower, support, heal and rethink breast cancer together. What statement below resonates most with your situation?
Scroll for more
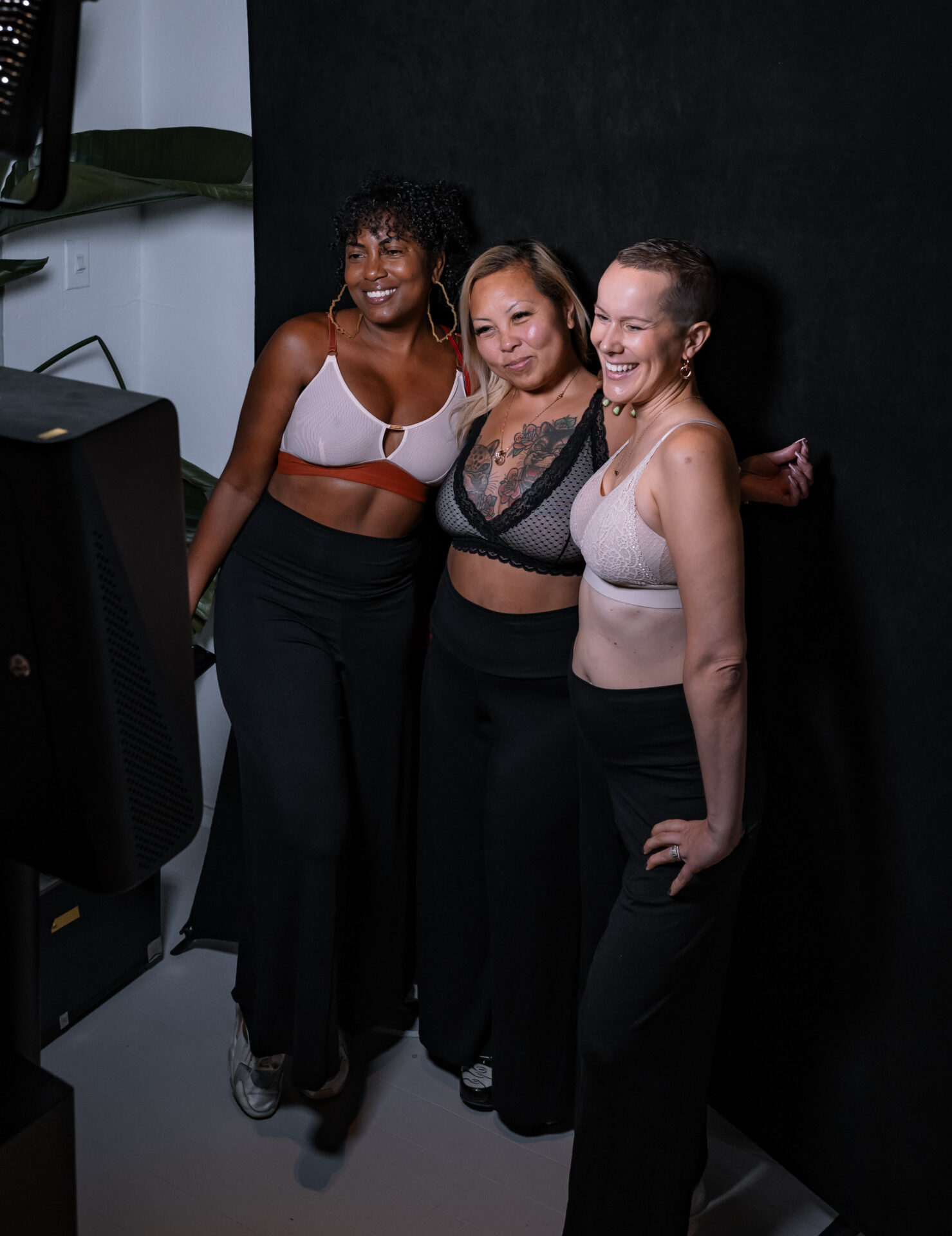



We are your breast cancer movement.
Rethink Breast Cancer educates, empowers and advocates for system changes to improve the experience and outcomes of those with breast cancer, focusing on historically underserved groups: women diagnosed at a younger age, those with metastatic breast cancer and people systemically marginalized due to other factors within the social determinants of health.